What to Expect During Perimenopause
Discover what to expect during perimenopause—from hot flashes to mood changes—and how to manage symptoms and stay healthy through your 40s and beyond.

By Monica Agar, MD, Obstetrician and Gynecologist—Virtua OB/GYN
For many women, the transition to menopause begins in the early 40s. Known as perimenopause, or the "menopause transition," this life stage is defined by a roller coaster of physical, emotional, and psychological changes. You'll know you've reached menopause when you haven't had a menstrual period for 12 consecutive months.
In perimenopause, your hormone levels fluctuate, and you may have symptoms you’d typically associate with menopause, such as:
- Periods that are heavier, lighter, shorter, or longer than you're used to
- One or more missed periods followed by a regular period
- Hot flashes, irritability, decreased sex drive, difficulty concentrating, and trouble sleeping
Think about when you hit puberty and got your first period—the change didn't happen all at once.
It's the same with perimenopause. You may see some of these changes in your early 40s or later. Every woman is unique, but here are some symptoms you may experience.
Perimenopause signs and symptoms
Menstrual cycle changes
It's important to know what a normal menstrual cycle is for you. Frequent bleeding, bleeding between periods, or prolonged bleeding may be perimenopause-related. However, if you have these symptoms, you should be evaluated by your OB/GYN.
Hot flashes and night sweats
Many women experience hot flashes, suddenly feeling a blast of heat from inside, followed by skin flushing and redness. Night sweats are similar, except you heat up when you’re asleep and wake in a sweat, which disrupts your sleep quality and ability to think and concentrate.
Mood changes, anxiety, or depression
As your hormone levels go up and down, so can your mood. You may experience anxiety, depression, racing thoughts, or find yourself easily irritated. There are many causes of mood changes, so it’s best to discuss your feelings with your OB/GYN or primary care provider.
Metabolism and weight changes
Weight gain and body changes are some of the most frustrating perimenopause symptoms. During this transition to menopause, your hormones start to dip, and your metabolism slows down. You may find that your weight gradually shifts from your hips and thighs to your waist, shoulders, and chest. Many women work hard to eat well and exercise and still can’t lose weight.
Meeting with a registered dietitian to discuss your nutritional needs during menopause can be helpful. You may also want to talk to a bariatric medicine specialist to see if weight-loss medication is right for you. Your doctor may also want to evaluate your thyroid levels to see if you may have an underactive thyroid, which contributes to weight gain.
Bone loss and osteoporosis
Perimenopausal estrogen loss can put you at increased risk for bone loss and osteoporosis, which can then lead to bone fractures as you age. Your provider can advise if you need supplements or medications to help you meet your calcium needs and maintain your bone strength.
Increased risk for other medical conditions
As you go through your 40s, your risk increases for conditions like heart disease, high blood pressure, and diabetes. During perimenopause, it's more important than ever to have regular medical checkups, vaccinations, bloodwork, and screening tests, including an annual pelvic exam and mammogram.
What to do if you’re experiencing perimenopause symptoms
It's always a good idea to talk to your health care provider about physical or emotional changes you may be experiencing. Even if they’re typical for this stage of life, it doesn’t mean you have to put up with them.
There are many hormonal and non-hormonal treatment options available for women at this stage of life. You can also improve your symptoms by making lifestyle changes, such as eating a diet rich in fruits, vegetables, low-fat dairy, lean proteins, and whole grains, doing weight-bearing exercises like walking or strength training for about 30 minutes a day, and reducing stress.
We’re here to help you manage perimenopause symptoms
- Find a Virtua OB/GYN near you and schedule an appointment online today.
- You deserve to feel like yourself again, and bioidentical hormone replacement therapy might be the solution. Call 856-325-5601 to schedule your consultation with Exuberan by Virtua.
- Learn about all your perimenopause and menopause treatment options.
There's So Much More to Explore
Discover expert insights, inspiring stories, health tips, and more by exploring the content below!

Discover How Robotic-Assisted Joint Replacement Surgery Can Benefit You

How Addiction Works: Causes, Signs, and Prevention of Substance Use Disorder

How to Tell the Difference Between a Minor Backup and Major Constipation

Managing Sarcoidosis: How Joann Found Relief Through Specialized Treatment

Choosing to Live in the Light: Simone's HER2+ Breast Cancer Treatment Journey

6 Ways to Support Healthy Blood Sugar in Teens

Managing an IBD Flare: Diet Tips to Reduce Irritation and Support Healing

Bioidentical Hormone Replacement Therapy Pellets: Relief for Menopause and Andropause Symptoms

HeartTalk Magazine

How to Recognize the Signs of Autism Spectrum Disorder in Children

Minimally Invasive Spine Surgery: Faster Recovery With Smaller Incisions

Zepbound for Sleep Apnea: A New Alternative to CPAP Therapy

New Technology to Light Tumors Helps Amy Overcome Lung Cancer

Early Ovarian Cancer Diagnosis: How Julie Trusted Her Instincts and Saved Her Life

6 Tips to Tame Your Spring Allergies

Debunking The Myths About Vaginal Dryness: Causes and Expert Treatment

Sex After a Hysterectomy: Timeline, Tips, and What to Expect

Bariatric Surgery Guide: FAQ on Recovery, Diet, and Weight-Loss Results

What Women Over Age 50 Need To Know About Late-Onset Lupus

Why Water, Fluids, and Protein Are Vital After Weight Loss Surgery

Your Diet Right After Bariatric Surgery

Your Diet Before Bariatric Weight Loss Surgery
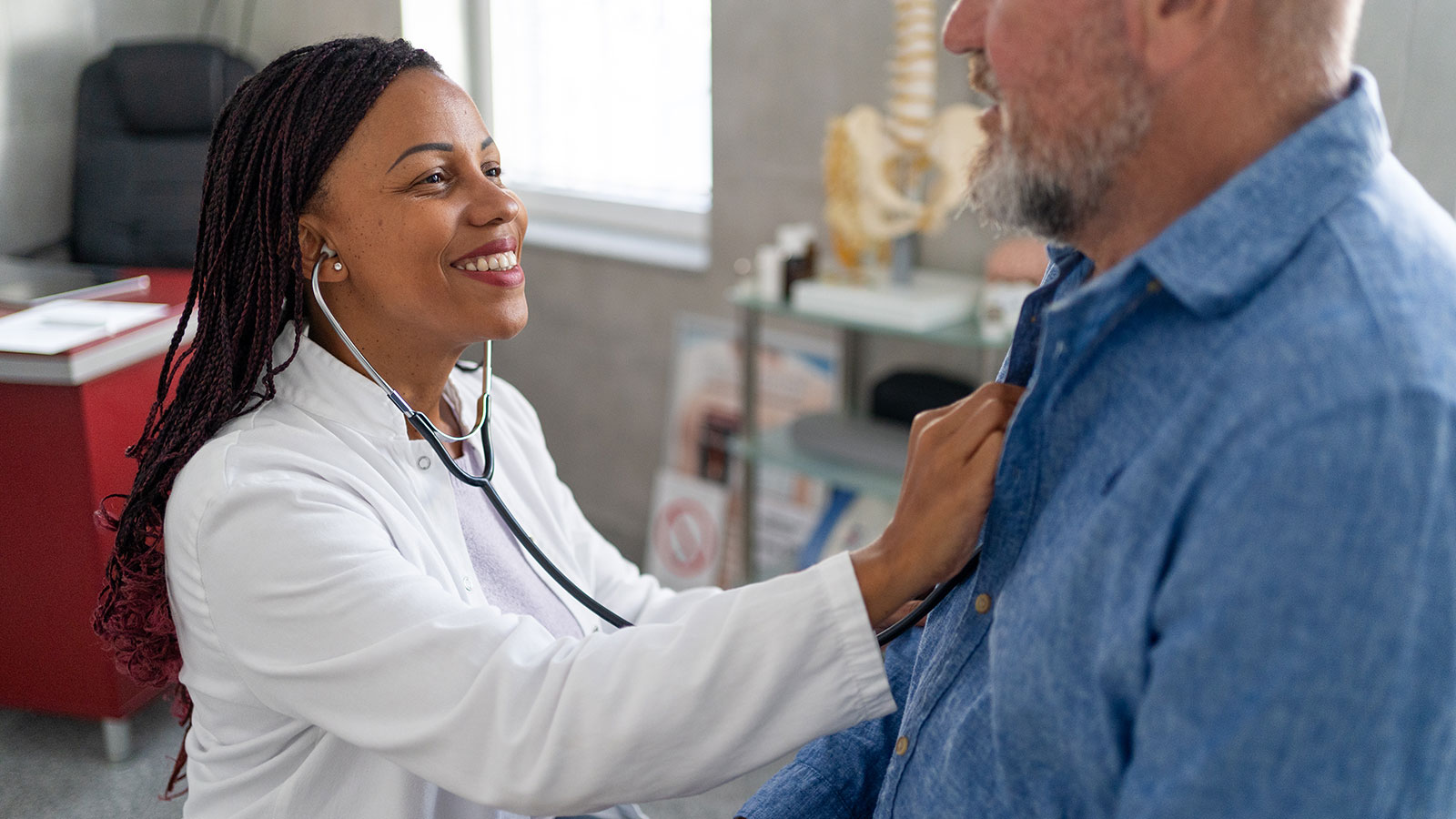
Heart Tests Your Doctor May Order

What Is SADI-S Surgery? A Guide to Loop Duodenal Switch Weight Loss Surgery

Colonoscopy and Robotic Colorectal Surgery Turned Patient's Worry to Relief

Are You At Risk For Chronic Kidney Disease
How to Reduce Inflammation to Lower Your Risk of Heart Attack and Stroke

Specialized Pregnancy Care for Thaysnara’s Cardiomyopathy

Weight-Loss Medications vs. Bariatric Surgery: What's Right for You?

Can Your Gut Health Affect Your Heart?

Benefits of Fiber: How to Increase Fiber Intake for Better Health

How to Use OTC Pain Relievers Safely: Acetaminophen vs. NSAIDs Explained

CASTLE Children's Mental Health Services Helps Josie Overcome Severe Anxiety and Regain Confidence

The Weird Pregnancy Side Effects No One Tells You About

At-Home Colon Cancer Tests vs. Colonoscopy: Which Screening Option Is Right for You?

8 Signs It's Time to See a Gastroenterologist

How the Unique Stages of a Woman's Heart Affect Her Health

Cervical Cancer Screening Guidelines: What You Need to Know

How to Spot the Early Signs and Symptoms of a Stroke

How Weight-Loss Surgery Can Improve Diabetes, Heart Health, and More

Knee Replacement Rehab: 7 Exercises to Restore Your Strength and Range of Motion

COPD vs. Asthma: Understanding the Difference in Symptoms

Why Is Sex Painful During Pregnancy? Pelvic Congestion Syndrome Explained

COVID-19 Vaccines and Pregnancy: FAQs

Don't Drink Alcohol? You Could Still Get Fatty Liver Disease

What Is the Difference Between Palliative Care and Hospice Care?

How to Exercise Safely with Asthma: Tips, Triggers, and Rescue Inhaler Use

How to Relieve Bloating Fast: Simple Tips for Quick Comfort

How to Tell the Difference Between Cold, Flu, and COVID-19

Jill Travels From Delaware to South Jersey for Advanced Lung Care

4 Exercise Tips to Help You Reverse High Blood Pressure

From Exhaustion to Empowerment: Tracy's Hormone Replacement Therapy Success Story

Why on Earth Am I Always So Cold?

Timely Heart Care During a Heart Attack Helps Joe Feed the Community

Allegra Is Thriving With Crohn's Disease

The Best and Worst Foods for Acid Reflux

How to Manage IBS Symptoms and Feel in Control Again

5 Types of Lung Disease: Symptoms, Causes, and Prevention Tips

Foods to Enjoy and Avoid for GLP-1 Heartburn

Sexual Health FAQs: The Questions Everyone’s Too Embarrassed to Ask

3 Reasons Why Now's the Time to Find Relief From Varicose Veins

Baseball Coach Turns Male Breast Cancer Surprise into Personal Mission

The Brain Health Checklist: 11 Questions Everyone Should Ask

From Caregiver to Patient: Robotic Surgery Relieves Teresa's Knee Pain

How to Get and Stay Healthy This Fall

How to Reverse Prediabetes and Prevent Type 2 Diabetes

Young Breast-Cancer Survivor Has New Hope for Healthy Future

What To Know About Vaginal Discharge During Pregnancy

Is Cancer Hereditary? What You Need to Know About Your Genetic Risks

Tara's Story: From Debilitating Uterine Fibroid Pain to a Half-Marathon Medal

Is Your Post-Pregnancy Belly Bulge a Sign of Diastasis Recti?

Your Guide to Mammograms: When to Get Screened and What to Know

Healthy Weight Gain During Pregnancy: A Guide for Moms-to-Be

IBS and Alcohol: Can You Still Enjoy a Drink?

Focus on Mental Health Is Key Part of Andrew's Weight-Loss Journey

What You Need to Know About Epilepsy

'Feeling Joy Again': ECT Brain Stimulation Therapy Restores Ashley's Well-Being

Not Just for Wrinkles: Botox Injections Promote Improved Bladder Control

Caring Maternity Team Transforms Harley's Pregnancy Crisis Into Lasting Memories

Robotic Hysterectomy, Trusted Care Help Bobbi Shine Again

How to Stay Cool and Prevent Heat Illness All Summer Long

What Happens to Your Body When You Don't Get Enough Sleep?

How to Have a Healthy Pregnancy if You're Overweight

4 Surprising Health Truths You Should Know

Is Low Sex Drive Normal? Revealing the Complex Causes of Low Libido in Women

CABG Surgery: What Women Should Know About Heart Health and Healing

Stress Incontinence vs. Urge Incontinence: What's the Difference?

5 Key Facts About Proton Therapy for Cancer Treatment

Mood Swings vs. Mood Disorders: Know the Signs and Get Help
Are emotional ups and downs disrupting daily life? Learn common signs of mood disorders, and when to talk to a doctor about diagnosis and treatment options.

4 Foolproof Pelvic Floor Strengthening Exercises for Women

What to Expect During Perimenopause

Protect Yourself From Tick Bites and Lyme Disease

4 Ways to Stay Fit and Healthy on a Budget

Do You Know the Signs and Symptoms of Uterine Fibroids?

How Are Uterine Fibroids Treated?

What to Expect From a Robotic Hysterectomy

When You Need A Hysterectomy Know Your Options

Take Control of Incontinence, Prolapse, and Other Pelvic Floor Disorders

How Can I Prevent Bone Loss and Osteoporosis?

How Do You Manage the Side Effects of Weight-Loss Medications?

A Woman’s Four-Step Guide to Fight Back on Back Pain
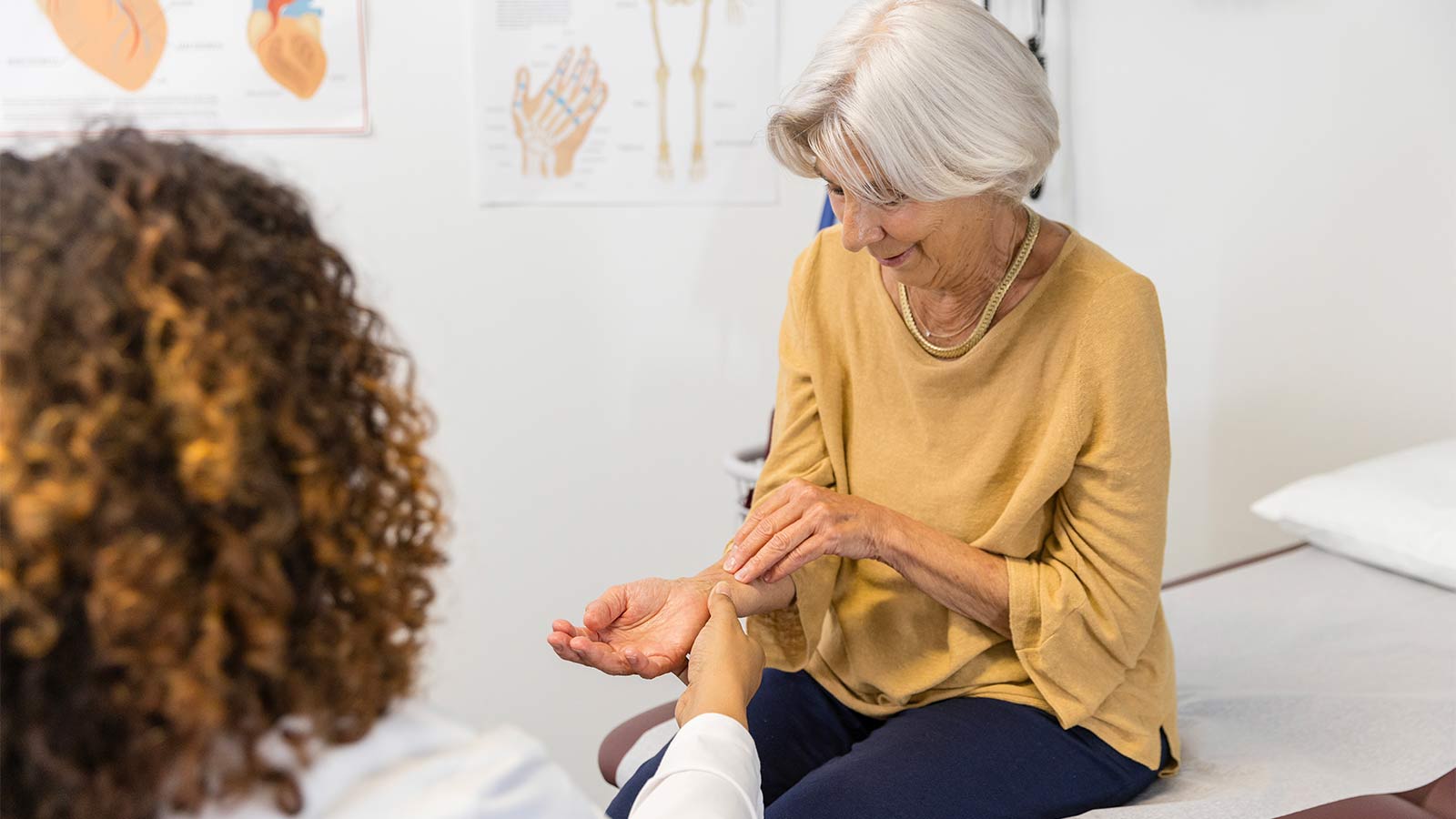
What You Need To Know About Carpal Tunnel Syndrome

The Truth About Menopause, Weight Gain, and Belly Fat

Shedding Light on Lesser-Known Menopause Symptoms and Solutions
Inside Look at Blood Vessels Aids PAD Treatment
Denise Davis: Pay Attention to Your Heart Health

What You Need To Know About Stroke Treatment

10 Smart Ways to Manage Your Diabetes

Signs You May Have Chronic Kidney Disease

5 Essential Winter Foot Care Tips When You Have Diabetes

Sweet Music: Trust, Teamwork Save Justin from Heart Attack

Advanced Minimally Invasive GYN Surgery Puts You at the Center of Care

Hepatitis C Kidney Transplant a Blessing For Lee Manns

7 Reasons Why You Want Your Surgeon to Be an Expert in Robotics

Colitis Symptoms Under Control, Jennifer Is ‘Living My Best Life’

How Do I Care for a Wound that Won't Heal?

Surprising Symptoms May Signal Stroke In Women

Five Back Pain Risk Factors That You Should Know
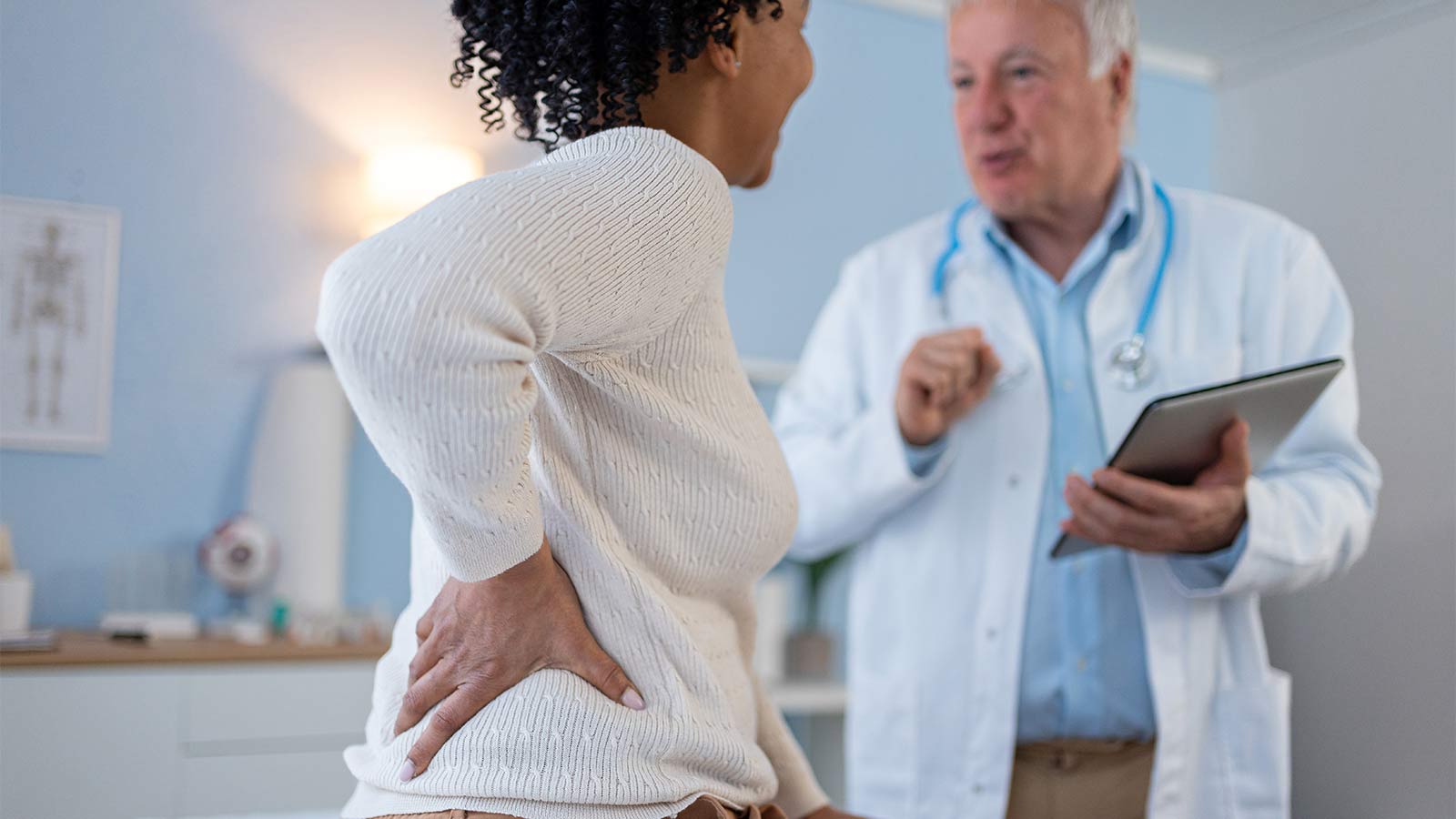
Is My Back Pain Normal, or Is It Spinal Stenosis?

Augmented-Reality Surgery Has Bobby Back on Stage, Rocking His New Hip

Robotic Hernia Surgery Combines Innovative Techniques With Faster Recovery Times

The HPV Vaccine: A Powerful Shield Against Cervical Cancer

How Does Breast Density Affect Your Mammogram?

Menopause: New Insights Into the Power of Hormone Replacement Therapy

How to Prevent and Treat Urinary Tract Infections

Signs You Should Get Treated For Vein Problems

One New Heart Valve Saves Two Lives in the Tritten Family

What You Need to Know About Heart Failure
Lung Valve Surgery Relieves COPD, Emphysema Symptoms

Lung Screening, Robotic Technologies Get Pat Kicking Up Her Boots Again

Breast Cancer Diagnosis Inspires Catherine to Help Others

Jasmine’s On-Air and Pain-Free After Gallbladder Surgery

When Should I See a Doctor About My Knee Pain?

Quick Action Leads to Jesse's Recovery From Stroke

A Non-Athlete’s Guide to Shoulder Overuse Injuries
Shoulder problems aren’t limited to athletes. Virtua orthopedic surgeon Sean McMillan, DO, explains shoulder overuse injuries and prevention in this article.

Put Lower Back Pain Behind You With This Ten-Step Guide
Wide-Awake Hand Surgery Speeds Recovery, Puts Control in Patients' Hands

South Jersey Veteran Thrives After Cross-Country Kidney Donation

3 Ways to Avoid Knee Pain

When Should I See a Doctor for My Hip Pain?

When Should I See a Doctor About My Shoulder Pain?

Is My Back Pain Normal, or Is It Sciatica?

Is My Back Pain Normal, or Is It a Herniated Disk?

When Is It Back Pain, and When Is It Something More?

Watchman Heart Device: a Technological Breakthrough for Blood Clot Prevention

Albert's Emergency Cardiac Surgery Is a 'Story of a Lifetime'

What Can I Do Right Now About My Aching Back?

How Do I Get Rid of This Back Pain for Good?

When Should I Be Worried About My Neck Pain?
Advanced Heart Failure Therapies Get Bernadine Back to Full Speed

Sarah Wins Back Her Health After Crohn's Disease Diagnosis

Overcoming Addiction, Philip Now Sees More Positive Side to Life
Firefighter's Successful Lung Cancer Care at Virtua
A Lung Screening Put Teresa Back in the Race

A Breast Self-Exam Saved Kristen's Life

How Sex Keeps You Healthy as You Age

Protect Your Child From HPV and Related Cancers

Why IUDs Might Be The Most Effective Birth Control

5 Things You're Too Embarrassed to Tell Your OBGYN

4 Not-So-Crazy Questions to Ask Your Doctor

Early Treatment is Best to Relieve Hemorrhoid Symptoms

The Top 10 Foods For A Healthy Diabetes Diet

Local Pastor Makes Kidney Health Mission of Ministry

What’s the Difference Between Type 1 and Type 2 Diabetes?

All for Bear: Dan Loses Weight to Be His Son’s Kidney Donor

Hyperbaric Wound Therapy Puts Joette Back in Motion

Robotic Hernia Repair Renews David's Active Lifestyle

